Advances in Vascular Surgery at Sunnybrook
The Division of Cardiac and Vascular Surgery at
Sunnybrook has recently recruited two young vascular
surgeons to their program with advanced endovascular
training.
Andrew Dueck, following his initial surgical training at
the University of Toronto in general and vascular surgery,
was recruited to Sunnybrook Health Sciences Centre in
2007 (http://www.surgicalspotlight.ca/Article.aspx?ver= Winter_2009&f=NewStaff). Following fellowship training
in vascular surgery in Toronto, he traveled to Phoenix,
Arizona to pursue advanced endovascular training under
Dr. Ted Dietrich at the Arizona Heart Institute (AHI).
AHI is a state-of-the-art facility designed to provide open
vascular, endovascular, and cardiac procedures together
in one location. There are four operating rooms each
equipped with C-arms for imaging, carbon fiber tables
and the full range of the latest devices and stents for cardiac
and vascular interventions.
"The dramatic changes required to train one individual
in such a broad range of skills would be disruptive
to current university training programs, the hospital
and the practice of vascular surgery and radiology, but
those barriers were never encountered. Wayne Johnston,
Tom Lindsay, Richard Reznick, Robin Richards and
Robert Maggisano made this unusual training regimen
possible. They just made it happen." Giuseppe Papia
has also recently pursued the Endovascular Fellowship
at the Cleveland Clinic. This is a high volume operative
fellowship available only to fully trained vascular or
cardiovascular surgeons. He was appointed to the group
at Sunnybrook this year. "Working together is an amazing
experience for us. We know that Drs Reznick and
Lindsay are doing things that we don't even know which
are facilitating our success."
At Sunnybrook, cardiologists, cardiac surgeons and
vascular surgeons had always worked under the administrative
umbrella of the Schulich Heart Program. The
question of which rooms could be used for hybrid cardiac
and vascular procedures was immediately answered
thanks to Brian Gilbert, head of the Schulich Heart
Program, and Eric Cohen, director of the cath lab. They were well aware of recent advances in the field of endovascular
surgery and were early and enthusiastic supporters.
"The cardiologists and cardiac surgeons helped us
build a centre that is equipped even better than the one
I worked in at the Arizona Heart Institute".
Andrew's colleague and office-mate Giuseppe
Papia (http://www.surgicalspotlight.ca/Article.aspx? ver=Summer_2009&f=NewStaff ) worked in two
dedicated endovascular suites for vascular intervention
in Cleveland. Overall there are 11 surgeons performing
hybrid procedures in five specially equipped rooms at the
Cleveland Clinic. Joe performed over 300 endovascular
procedures "from skull base to the toes with every possible
device available that you can imagine." There he
worked with Roy Greenberg, a pioneer and world expert
in branched aortic endovascular aneurysm repair (EVAR)
for thoracoabdominal aneurysms. At the Cleveland Clinic
they performed three to five of these complex cases per
week. "The team spirit and efficiency at both of these
centres was outstanding. If the surgeon is seen as the lead
paddler of the canoe there was never anyone behind dragging
a paddle or an anchor -- the rest of the team provided
an outboard motor. Turnover time was generally eleven
minutes. The dress code in the Cleveland Clinic operating
room simplified communication. Staff surgeons wear
white, residents wear blue and industry representatives wear
orange. Everyone on the team takes great pride in the clinic
and patients feel the esprit de corps."
Endovascular procedures are not new. Joe and Andrew
emphasize that their vascular radiology colleagues have
been performing angioplasty since the 1980s, and endovascular
stenting for abdominal aortic aneurysms has
become the standard of practice throughout Canada.
They are now pushing the envelope in terms of more
complex hybrid interventions such as endovascular-aortobifemoral
procedures, and catheterization through patches
over profundoplasties to facilitate the introduction of
balloons and stents in both directions. For example this
allows "aorto-bifemoral bypasses" to be performed with
two small groin incisions. These multilevel interventions
allow patients to go home quickly, often in one to two
days. More importantly they are spared the long period of
recovery at home associated with open procedures. "The
novelty is not choosing one or the other, open or endo,
but being able to combine the best of both endovascular
and open surgery for each individual patient. As the specialty
evolves, the surgeons must also evolve. Daryl Kucey
and Robert Maggisano were the pioneers at Sunnybrook
who broke the ground with the radiologists, raised money
for the equipment and the cardiac surgeons and cardiologists
at the Schulich Centre. Dr. Maggisano became a
tireless fundraiser, sharing his vision with a broad range of potential donors. Major donors became infected with
|
Dr. Maggisano's contagious enthusiasm, bought into the vision early and offered financial support, which in turn encouraged additional donations. These efforts enabled the purchase of the initial equipment. Brian Gilbert and Eric Cohen provided key administrative support to developing additional infrastructure. The diaphragm and the heart lung machine are no longer defining boundaries between vascular and cardiac surgery. These two surgical specialties have been one division at Sunnybrook for the past four years, and collaborate to perform cases in a combined fashion. There is a strong relationship with the division of cardiology with Drs. Madan, Dick, Strauss, Cohen and Radhakrishnan all playing an active clinical and research role. Most recently, the cardiac surgeons, cardiologists and vascular surgeons have come together to form a team for the performance of transfemoral aortic valve surgery.
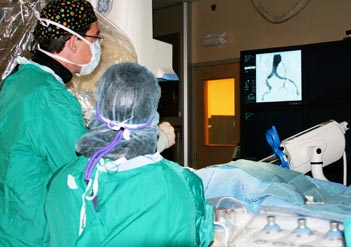
Endovascular Suite at Sunnybrook
|
In addition to the multilevel collaboration amongst
specialties in the operating room and endovascular suites,
Joe's presence in the cardiovascular ICU also helped bond
the services together. He has especially good rapport with
surgeons in the ICU and when attending in the ICU has
helped nonsurgical staff understand the unique culture
and values that inform post-op surgical care. Everyday
at the Heart and Vascular Institute at Cleveland Clinic
Foundation there are different trans-disciplinary rounds
that build team cooperation. Tuesdays -- vascular medicine
and surgery, Wednesdays -- aortic rounds with the
cardiologists and cardiac surgeons, Thursdays -- carotid
rounds with all disciplines including neurosurgery. "These
provided an incredible educational forum where different
disciplines treating the same disease discussed cases
and approaches together. The spirit was that the patients
belonged to the Clinic, not individual physicians, therefore
everyone worked together to ensure they received the
best treatment possible."
The Trauma service is another important area of synergy
at Sunnybrook. "The trauma surgeons are excellent
at vascular repair. They call the vascular surgeons only
for replacement, bypass or reconstruction of unsalvageable,
unrepairable vessels. It helps that we are friends
who trained together and that they are so good at what
they do."
The research agenda is a collaborative one. Andrew
is working with Graham Wright and his imaging sciences
group, a well-funded and productive research team
developing measurement tools to replace older standards
familiar to many surgeons such as the anklebrachial index.
These measurements will introduce techniques that will
allow assessment of microvascular disease essential to
determine and predict the fate of more proximal interventions,
and potentially a mechanism to evaluate stem cell
therapies. Other important collaborative research includes
the quest for developing non-contrast imaging for renal
patients, a 3-dimensional model of the vascular tree using
intravascular ultrasound that looks forward rather than
only at cross-sectional images, and translational research
to be sure that the advances in understanding and treatment
are brought to the population throughout the province.
Joe's research is focused on his background in intensive
care and his interest in patient safety and minimizing
harm to patients through the standardization of process.
With the support Rob Fowler and the Department of
Critical Care Medicine, and Robin Richards, Joe has
recently completed training at the Institute for Healthcare
Improvement in Boston with Dr. Don Berwick and his
team. "Don Berwick is probably the most respected physician
in America and an absolutely inspirational speaker
when it comes to patient safety. Escape Fire: Lessons for the
Future of Healthcare is a must read for anyone who takes
care of patients." His focus is on standardizing process for
"handovers"-- the critical points in the care cycle where
everything can potentially go wrong for patients. He is
working on a formal process for handing over patients
from the Operating Room to the ICU. He works in the
Patient Safety Scholar program with Ed Etchells and
Kaveh Shojania. Joe is also currently piloting and working
on the implementation of the WHO Surgical Safety
Checklist at Sunnybrook's two sites, and is working with
the provincial SSCL working group. He is collaborating
with Sherry Espin, Associate Professor of Nursing at
Ryerson University, on evaluating the implementation
process of the WHO checklist across the province as well
as it's effect on operating room culture.
M.M.
|